Vitrectomy
What is Vitrectomy?
Vitrectomy is a surgical procedure undertaken by a specialist where the vitreous humor gel that fills the eye cavity is removed to provide better access to the retina.
How is Vitrectomy Performed?
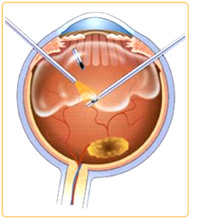
Vitrectomy surgery is typically done in an operating room using a vitrectomy machine and operating microscope. Tiny openings are created in the white part of the eye (sclera) 3-4 millimeters posterior to the limbus (pars plana). Specialized micro-instruments are inserted into the vitreous gel through the openings in the sclera and the vitreous gel is cut out. Other micro-instruments can be used to remove scar tissue and apply laser to the retina.
Specialized saline, gas or silicone oil is injected into the eye to replace the vitreous gel at the end of the surgical procedure. Using of small gauge 23-gauge and 25-gauge instrumentation in vitrectomy surgery is a current standard of care and don't needed a conjunctival opening and suturing.
When is Vitrectomy Performed?
-Diabetic retinopathy
-Vitreous hemorrhage
-Epiretinal membrane
-Macular hole
-Retinal detachment
-Retinopathy of prematurity
-Cataract surgery complications
-Endophthalmitis
-Severe eye injury
Last Updated: October 23, 2024














